Dieser Beitrag ist auch verfügbar auf:
Deutsch
The contents of our interview:
- Up to 45% of dementia cases can be delayed if we take the risk factors seriously
- Why dementia is often not diagnosed at all or is diagnosed far too late
- At what point should you seek medical advice?
- What do I do as a family caregiver if potential patients do not want to be examined?
- How do blood tests that provide indications of Alzheimer’s disease work?
- Which medications can help in everyday life after a diagnosis?
- Genetic tests that indicate a higher risk of developing dementia later in life: How reliable are such tests and where are they used in practice?
Dementia is not only a medical diagnosis, but also a social challenge: In Austria, around 170,000 people are currently estimated to be affected, in Germany around 1.8 million. Forecasts for both countries predict that these figures could almost double by 2050.
Nevertheless, the true extent of the problem can only be estimated. This is because dementia is still often not diagnosed at all, or only very late — and thus often only after valuable time has already been lost. Large-scale studies show that prevention can significantly reduce the risk. And early diagnosis can help delay the onset of symptoms and ensure that the right support is organized in a timely manner.
We’re discussing these strategies with Dr. Sara Silvaieh, a dementia expert at the University Clinic for Neurology at the University of Vienna, and Raphael Schönborn, an expert on dementia, delirium, and brain health. What can medicine realistically achieve today? And above all: What can each of us do to stay healthy for as long as possible? A conversation about prevention, early detection, and the courage to take action at the first sign of trouble.
SBC: Many interviews emphasize that we have a lot in our own hands – and to a certain extent can help determine how healthy we stay in old age. What factors increase the risk of developing dementia and what specific measures help to realistically reduce the risk? Can we prevent dementia?
Dr. Silvaieh: Based on current knowledge, dementia cannot be completely prevented. But there are steps we can take to reduce the risk and delay its onset. Large-scale studies show that up to 45 percent of dementia cases can be delayed if we take the risk factors seriously.
There is just no one trigger, usually several factors come together. A small part is genetic and therefore cannot be influenced, but this form is rather rare. The greater leverage lies in things that we can control in everyday life. Exercise plays a major role: For example, around 5,000 steps per day are cited as a guide; more exercise can further increase the effect. Diet also counts: A Mediterranean, healthy diet – i.e. less animal fats, eating more consciously overall and eating fish once a week, for example – is considered beneficial for our brain.
Two points are uncomfortable but important: Smoking and alcohol. Smoking is a very strong risk factor and it is recommended that you stop. When it comes to alcohol, the current recommendation is to drink as little as possible. The earlier idea that a glass of red wine is generally good for the heart and brain is now viewed much more cautiously. It is also worth paying attention to traditional health values: High blood pressure should be detected early and treated well, and cholesterol levels and check-ups are also relevant.
Hearing and vision are also often underestimated. Those with impaired hearing should use hearing aids; those with impaired vision should wear glasses. This is not just for comfort: When perception is impaired, mental and social activity often decline too – and this can put additional strain on memory. It is important to remain cognitively active: Stay curious and engaged, challenge your brain.
The best time to start is ideally from the middle age of around 40 at the latest. Earlier is always better, but later still brings benefits. And another important addition: The 45 percent figure is a value from studies. This is no guarantee for the individual person – even those who do a lot of things right can still fall ill. But the data shows: If many people reduce their risks, a large number of dementias in the overall population can be postponed significantly. The aim is to pay attention to all risk factors, grow older in a healthy way and thus protect our cognition and memory.

SBC: Mr Schönborn, you emphasize in your presentations that dementia is often not diagnosed at all or only diagnosed very late. In your opinion, why is it that warning signs are so often overlooked or suppressed – and that we therefore lose valuable time to influence the course of the disease at an early stage?
Schönborn: Many diagnoses are made so late because dementia is still strongly associated with fear, shame and a stigma in our society. Anyone who suspects that something is changing faces a double hurdle: on the one hand, the idea of dementia seems like a frightening image. On the one hand, the idea that you are losing your mind and can’t do anything about it dominates. Furthermore, those affected often experience that they are treated differently after open communication. As a result, many people prefer to ward off, deny or avoid the topic. Not necessarily because they don’t notice the changes, but because it is difficult to integrate it into their own self-image.
On top of that, the prevailing narrative has long been that there is nothing that can be done about dementia. If a diagnosis is perceived merely as a final verdict, people are less motivated to seek an early evaluation. Yet early evaluation is crucial— also because there isn’t just one type of dementia but different forms and, in some cases, treatable causes, provided they are detected in time. Even if medication cannot halt the progression of the disease, it can still have a positive effect, depending on the form and stage of the disease. Above all, however, one thing is certain: denial does not solve problems; it usually makes them worse—for both those affected and their loved ones.
SBC: What are the signs that make it worth investigating? What is normal forgetfulness and when should a disease be investigated?
Dr. Silvaieh: Basically, it is quite normal for us not to remember a name in a stressful situation. Especially if you remember it later and it doesn’t happen all the time, it’s usually nothing to worry about. However, you should take a closer look if forgetfulness affects your everyday life. For example, if bills are repeatedly not paid, if appointments suddenly have to be constantly noted down even though this was not necessary in the past. Or if the same questions are asked again and again, even though they have already been answered.
Frequent word-finding problems can also be noticeable. Not the occasional “What’s that again?”, but when sentences regularly break off or can no longer be completed in a meaningful way. Changes in social behavior can also be a signal: Some people withdraw because they find conversations in larger groups difficult or because they notice that they lose the thread more easily – and this can then lead to social isolation out of shame.
In medical terms, dementia is primarily defined by the fact that memory problems persist over a longer period of time and lead to restrictions in everyday life. A distinction is made between more complex everyday activities such as shopping, telephoning, taking and managing medication or housekeeping – and basic activities such as personal hygiene, getting dressed or eating. If the more complex things become more difficult first, this may be an early stage; if basic activities are already affected, this indicates a more advanced stage.
It is important to note that even though the formal diagnostic criteria often speak of at least six months, nobody has to wait that long. If relatives or those affected notice significant changes after just a few months, it makes sense to seek clarification early on – from your family doctor, a neurologist or a memory clinic. After all, it doesn’t always have to be dementia: there are also treatable causes of memory problems, such as a pronounced hypothyroidism or other medical reasons. That’s why it’s worth looking early – not out of panic, but to get clarity and the right treatment.
SBC: As a family caregiver, what should I do if potential patients refuse to get tested? What should I do?
Dr. Silvaieh: If an affected person doesn’t want to get a check-up, it’s often not due to stubbornness, but to shame, fear and the fact that they don’t always understand their illness. In such situations, it usually doesn’t help to put pressure on the person or to immediately use the word dementia. It makes more sense to start with a low-threshold approach: Don’t talk about a diagnosis, but about clarifying whether there is a treatable reason for the memory changes. Many causes are actually treatable or at least easy to influence, for example diabetes, thyroid problems, vitamin B12 deficiency, side effects of medication or other medical triggers. This perspective often removes fear and increases the willingness to take the first step.
Sometimes a very specific, personal motive can also help to persuade someone to seek clarification – for example, the desire to continue driving safely. The key is to find out what is important to the person and to build on this. This is very individual.
In practice, it has proven useful to start small and build on existing trust: first visit your family doctor, where a blood test, a medication check and a short memory test are possible. Ideally, you should be accompanied by someone who can describe the changes in your everyday life. This is because self-perception and the view of relatives often differ.
If there are any abnormalities, the patient is usually referred to neurology or a memory outpatient clinic. There, basic diagnostics are carried out, primarily to rule out other causes. This usually includes an MRI scan of the head, for example to clarify undetected strokes, other structural causes or rarer triggers. A detailed neuropsychological test is also carried out. Depending on the results, further detailed diagnostics may follow, such as special examinations to confirm Alzheimer’s disease more precisely. Suitable therapies and support can then be initiated at the same time.
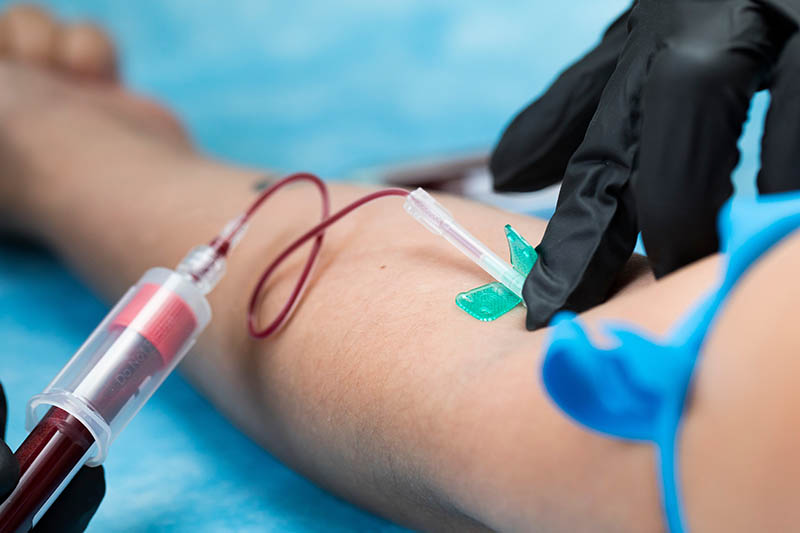
SBC: There are now blood tests that can provide indications of Alzheimer’s disease. How does such a test work in practice and where can I have it carried out?
Dr. Silvaieh: Blood tests for diagnosing Alzheimer’s disease are currently considered one of the most exciting developments in diagnostics. In Alzheimer’s disease, certain proteins—primarily amyloid and tau—accumulate in the brain. Biomarkers can provide evidence of these disease-specific changes. Until now, such changes have primarily been detected through amyloid PET scans or by analyzing cerebrospinal fluid. (Note: A PET scan is a positron emission tomography scan that can visualize changes in the brain—such as amyloid deposits in Alzheimer’s disease.) While a conventional MRI can provide indications of more advanced changes, it may still be unremarkable, particularly in the early stages. An unremarkable MRI therefore does not rule out early-stage Alzheimer’s disease.
Blood-based biomarkers therefore represent an important step forward. They are currently seen primarily as a complementary component – especially in people who already have initial memory changes or other abnormalities. However, it is crucial that such tests are classified by specialists and embedded in a comprehensive diagnostic process.
Self-organized testing without medical supervision is currently not recommended. The results are often difficult to interpret, especially in healthy individuals, which can lead to uncertainty rather than clarity. The current recommendation is therefore: blood tests can play an important role in the future, but should currently be used in a targeted manner and as part of a medical assessment.
SBC: After clarification – which medications can help in everyday life and how do they work?
Dr. Silvaieh: In the long term, a certain neurotransmitter in the brain is important in Alzheimer’s dementia: acetylcholine. It supports our memory and thinking. Many drugs used to treat Alzheimer’s have precisely one aim: to ensure that acetylcholine is broken down more slowly so that the brain has more of it available for longer.
In practice, however, there is sometimes a catch: some medications work in exactly the opposite direction. They are called anticholinergic and can impair memory performance in the long term. This is particularly common with drugs for bladder weakness or an overactive bladder, but also occurs with certain allergy medications and some antidepressants.
Many people take a lot of medication at the same time over the course of time. In the outpatient memory clinic, we often see lists of twelve or thirteen preparations. We don’t always check in detail whether there are any interactions or whether a medication has an additional negative impact on memory. That’s why it can be very helpful to regularly sort through all the medication: What is really necessary, what is it being taken for, and where can you simplify or better coordinate? Above all, it is important to take a conscious look at the list of medications and check for interactions.
And regardless of this, even if a diagnosis is made, the familiar adjustments remain important: adjust blood pressure and cholesterol, reduce excess weight, don’t smoke, keep alcohol to a minimum, compensate for hearing and vision problems, have depression treated and remain mentally and socially active. Protection against head injuries also plays a role, for example by wearing a helmet when cycling. Even environmental factors such as air pollution are now being discussed as a possible influence.
SBC: In addition to the question of whether dementia is already present, there are also media reports about genetic tests that are supposed to indicate an increased risk of developing dementia later in life. What is the current state of knowledge on this, how reliable are such tests and where are they used in practice?
Dr. Silvaieh: Such tests are not a simple precaution like a blood count – and they are not used to test healthy people simply out of concern. What is possible and useful in practice is a clarification if there are specific changes or if there were very early illnesses in the family. This is because many dementias are not diagnosed at all or only at a late stage, and not all those affected appear in statistics. This makes a clear, pragmatic approach to clarification all the more important.
If there was dementia in your family and it started very early – as a guide: before 65 – the risk of a rare, genetic form may be higher. These hereditary forms of Alzheimer’s are generally rare and often appear very early – sometimes as early as around the age of 40. In such cases, the person affected – e.g. the mother – is usually genetically tested first. Only if a corresponding genetic mutation is actually found there can we even discuss whether a healthy family member would like to be tested. However, this is not a normal test, but a sensitive process with mandatory counseling and psychological support, because the result can have a major impact on life planning.
If there are no genetic findings in the affected person, genetic testing is not usually carried out on healthy relatives. And if you are only concerned without any symptoms of your own, genetic testing is also not planned in the clinical setting.
What does this mean in concrete terms if you want such a test? The best first step is usually to see your family doctor. If there are any indications after the initial basic examination, a specific referral can be made, for example to a neurologist or a memory outpatient clinic. Depending on the situation, a decision will then be made as to which tests are appropriate. Blood tests can play a role here, but these are usually embedded in a medical assessment – and not as a quick test without context.
SBC: Mr. Schönborn, as Managing Director of PROMENZ, you support affected people and family caregivers. Dementia is on the rise: in your opinion, what would be the next step to help these people?
Schönborn: There is currently a lack of translation between the message – you can do something – and the reality: it is increasingly being emphasized that prevention is possible and that you can exert influence. But at the same time, there is a lack of low-threshold services in many places that address, educate and support people at an early stage.
This is exactly where self-help groups and advice centers come in: They enable quick support, provide relief, help with classification and create spaces where people can talk openly. If we want diagnoses to be made earlier, we need not only information, but also attitude, language – and easily accessible structures that do not leave those affected behind.
Thank you very much for the interview!
The next online discussion with Raphael Schönborn and Dr. Silvia Silvaieh will take place on World Alzheimer’s Day, September 21, 2026, from 5:00 to 6:30 p.m (in German). Topic: Advances in prevention, early detection, and treatment – hopes, opportunities, and facts. You can register here: https://kompetenzdemenz.at/weltalzheimertag/
Author: Anja Herberth
Chefredakteurin

















